Why Antibiotics Don't Help Winter Viruses

Every week in winter, Rospotrebnadzor (the Federal Service for Surveillance on Consumer Rights Protection and Human Wellbeing) reports which ARVI (acute respiratory viral infection) Russians have contracted. And the same infection names appear in the reports time after time. Our colleagues from 63.RU decided to figure out how all these viruses are similar and different. They also learned whether superinfections really occur or if it«s just scare stories. And whether we should expect a second flu epidemic.

These and other questions were answered by the chief freelance infectious disease specialist for Samara, head of Infectious Diseases Department No. 2 at the Clinics of Samara State Medical University, infectious disease doctor Yekaterina Kindalova.
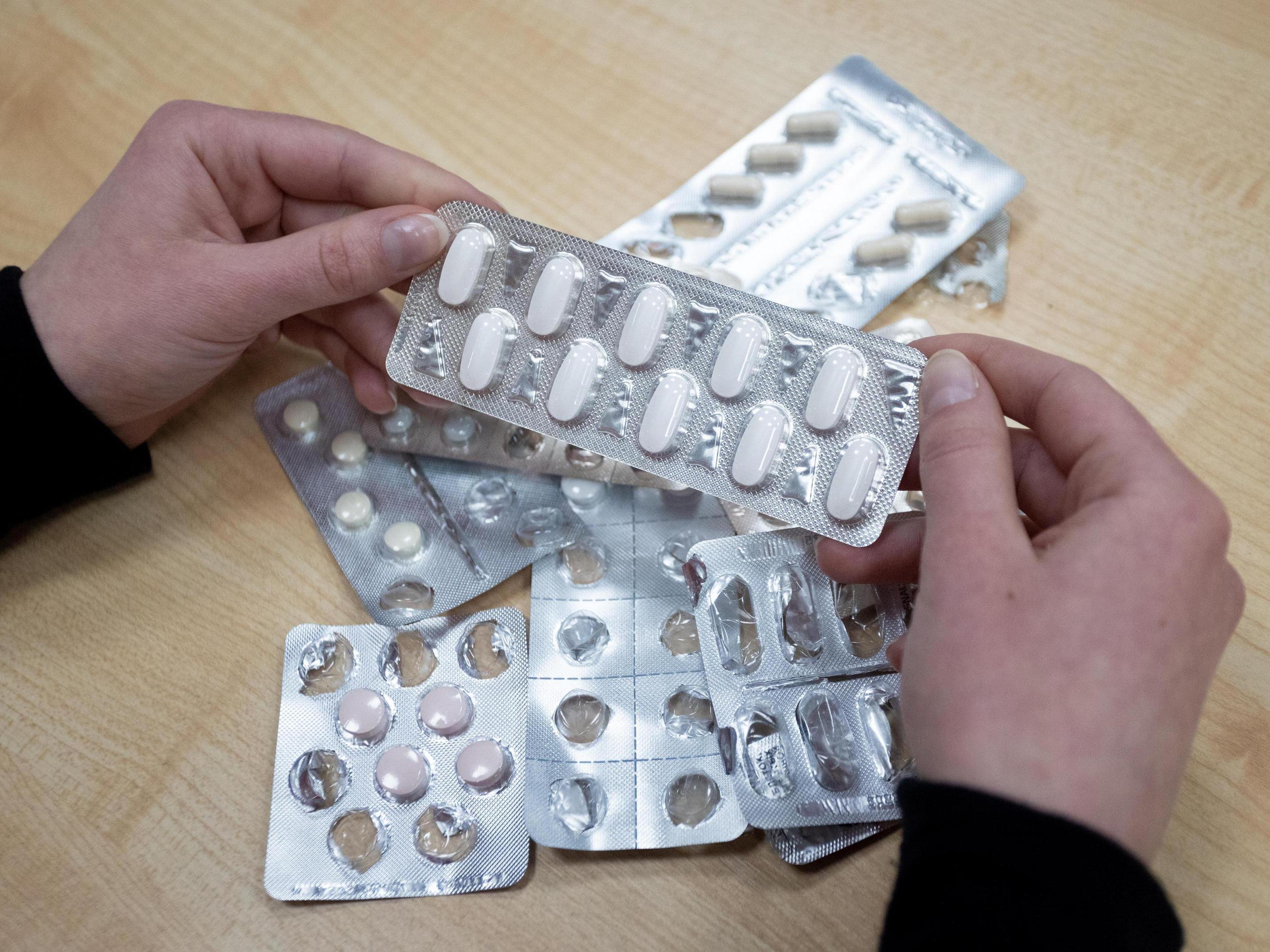
Without a Swab, It«s Hard to Tell
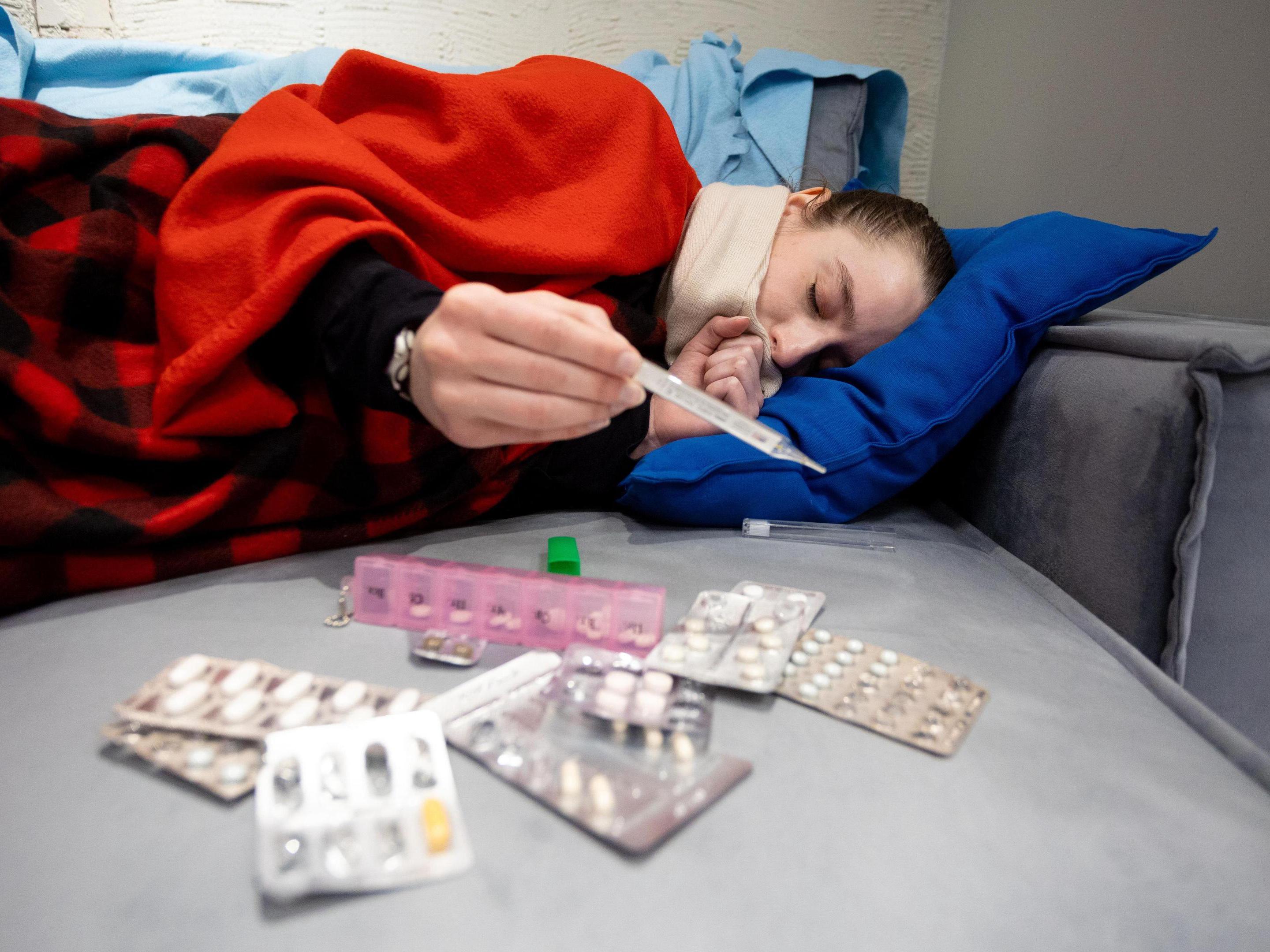
— Rospotrebnadzor reports that Russians are most often contracting parainfluenza, adenovirus, RSV, metapneumovirus, rhinovirus, and COVID-19. We«d like to examine the specifics of each of these viruses. How are they similar and different?

— The reports from Rospotrebnadzor are unsurprising. Autumn, winter, and early spring are the traditional times when respiratory viruses surge. There are more than two hundred different ones; you listed those that are most common here.
It probably makes little sense for the average person to distinguish them because they are similar. Sometimes even a primary care physician cannot say for sure without laboratory confirmation what you have. All these viruses will typically cause fever, signs of intoxication (weakness, malaise, muscle pain), and some damage to the respiratory system.
For some viruses, their main manifestations are clear from the name. For example, rhinoviruses. Rhinos means nose — these are the most common viral infections, up to 40% of all pathologies. The leading symptom is rhinitis, a runny nose.
Parainfluenza affects the larynx, manifesting as laryngitis with a rough, dry, barking cough. In children, laryngitis is more often complicated by laryngeal stenosis — one of the main reasons children are brought to pediatric or infectious disease hospitals.
Adenovirus affects glandular tissue: lymph nodes enlarge, eyes become affected, causing conjunctivitis, sore throat, and tonsillitis.
Respiratory syncytial virus (RSV) mostly affects the lower respiratory tract. In children, it often presents as bronchiolitis.
Metapneumovirus mostly affects children, and clinically it resembles influenza. So I repeat: without laboratory confirmation — without a swab from the nose or throat — we cannot always say for certain, «Yes, you are sick with this particular virus.»
How to Treat
— Are these viruses treated differently? Or are the medications similar?
— Specific therapy exists only for the influenza virus (I«m referring to drugs with a direct effect on the virus). For all other viruses, no such therapy has been developed, and treatment is symptomatic. For example, bed rest during fever, plenty of fluids, nasal rinsing, vasoconstrictor nasal drops, and throat care if there is pain.
— Concerning antiviral drugs: when should they not be used, and when are they absolutely necessary?
— All antiviral drugs are most effective when taken early, within the first 48 hours — ideally within 24 hours — of symptom onset. After that, they lose the effectiveness we would hope for. And, of course, these drugs should only be taken as prescribed by a doctor.
What we can do without a doctor«s prescription is take an antipyretic, use vasoconstrictor nasal drops if congested, monitor our condition, and keep an eye on any underlying conditions. For example, patients with diabetes should carefully monitor blood glucose levels, and those with blood pressure issues should monitor that.
Every patient can do this at home, but they should never prescribe antiviral drugs to themselves, because these medications have both indications and contraindications.
— Can you name a few typical mistakes people repeatedly make when trying to treat themselves, despite all recommendations?
— First, continuing to go to work or school with clinical symptoms like cough, runny nose, and fever. Not only are they sick themselves, but they also infect people around them. So during the period of pronounced clinical symptoms, it«s better to stay home.
Second, of course, is self-prescribing antibacterial drugs (antibiotics). For viral infections, they are absolutely useless and do nothing because the pathogen is a virus, not a bacterium. And in some cases, they can even be harmful because they affect a person«s own microbiota, both in the respiratory tract and the intestines.
I would also mention the overuse of antipyretics and nonsteroidal anti-inflammatory drugs. When recommended dosages are exceeded, it can lead to quite adverse consequences.
«We Don»t Get Sick Just Because We Got Our Feet Wet«
— Can a person understand for themselves whether they caught a virus or just caught a cold? For example, their throat hurts, and the day before they got their feet wet.
— We don«t get sick just because we got our feet wet. We get sick when some pathogen enters our body. Or if a person has chronic issues, such as chronic tonsillitis or longstanding tonsil problems. The fact of hypothermia can activate the pathogenic flora that was already present in the person — they were just keeping it under control. So we need to figure out what the cause is and what the pathogen is.
— Is it possible to be infected with several types of ARVI at the same time? I mean the so-called superinfection that has been talked about recently.
— Yes, that is possible. For example, during the pandemic, we saw patients who were simultaneously infected with both influenza and COVID-19. So catching several viruses at once is entirely possible, since they circulate simultaneously.
— What would the clinical picture look like then? Would one virus dominate with stronger symptoms, or would the person be immediately hit with fever, sore throat, runny nose, and nausea all at once?
— It depends on the amount of pathogen that entered the body. The clinical picture of one respiratory illness might come to the fore. Alternatively, it might be completely unclear what the person has, with different manifestations from different organs and systems. Here, laboratory diagnostic methods come to our aid again.
But as a rule, these patients are sicker and more often require hospitalization, sometimes even intensive care measures.
— Have superinfections become more common recently? Or has diagnostics simply improved?
— After the encounter with the coronavirus infection, when the approaches to organization were revised and filters and isolation boxes were set up, we gained more diagnostic capabilities; we have rapid tests for different viruses. We detect and diagnose more.
— What is the current situation with COVID-19 incidence?
— COVID-19 is not as common now as it was in 2020–2021, and it has changed. Fortunately, we very rarely see patients with severe cases and extensive lung damage now.
We see quite a lot of adenovirus infection and parainfluenza.
— A question about the super virus. Doctors are now talking about a possible epidemic of some kind of super virus — a mix of monkeypox, rubella, bird flu, and Oropouche fever. Is an epidemic of such a super virus threatening Russians?
— «Super virus» is more of a non-medical term. In medicine, epidemiologists and infectious disease specialists have the concept of «X-agent» — some unknown agent that could potentially emerge.
The risk of a new pathogen emerging certainly exists. All systems are carefully monitored, as are all emerging outbreaks. So I think in the near future we won«t face anything serious in Russia.
— Respiratory viruses circulate most often in winter. What about spring?
— In summer, late spring, and early autumn, it«s intestinal infections: enterovirus, norovirus, rotavirus. Although they do occur throughout the year now, incidence is certainly higher in warmer periods.
«Influenza Virus Doesn»t Like Dry, Frosty Weather«
— And why is that? Because respiratory viruses spread better indoors, in cold weather, and in dry air?
— Each virus has different conditions in which it feels comfortable — different temperatures and humidity. In winter and autumn, we are in crowded groups: everyone has returned from vacations to work, school, and daycare. And weather certainly plays a role, although the influenza virus, for example, doesn«t like very cold, dry weather. It reproduces more actively when it»s more humid and around -10°C to -15°C (14°F to 5°F). That«s better for it than dry, frosty weather.
— There is information that we are expecting another epidemic in February — this time influenza B. Do such forecasts really exist?
— As a rule, influenza B does not cause such large outbreaks, so there are no forecasts of a total epidemic. Influenza A (H3N2) is actively circulating now. Influenza B was and is included in the vaccines that the population received in autumn. So I still hope there won«t be a large outbreak.
— If a person has had influenza A, could they potentially get influenza B?
— Of course.
— What preventive measures are there? Obviously, if someone wanted a flu shot now, it«s too late. How can we protect ourselves from flu or other ARVI right now?
— Maintain social distancing — something we all learned during the coronavirus pandemic; wear masks in crowded places; don«t touch your face or rub your eyes; use hand sanitizers. If someone is already sick, it»s better for them to stay home. Other recommendations: lead a healthy lifestyle, which includes adequate sleep, stress reduction, walks in the fresh air, exercise, and a balanced diet.
I would like to say that vaccination currently — particularly against influenza — is the most effective, safe, and fortunately accessible way for our population to prevent this disease, avoid major problems later: severe illness, complications, and death. So we shouldn«t forget about vaccinations. And it»s best to get them in September or October, because after any vaccination, the body needs time to produce antibodies and build protection.





